Molar evacuation
Suction evacuation is recommended for complete and partial molar pregnancies. If evacuation is followed by excessive bleeding, a single dose of oxytocin can be used after complete evacuation.
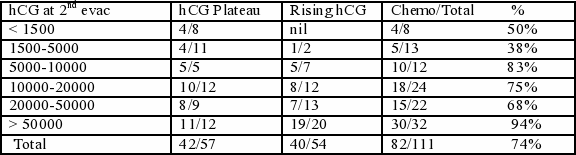
For persistent disease repeated evacuations bring reducing results and repeated procedures are rarely advised. We suggest referring teams discuss this with CXH prior to repeated evacuation. The table below shows the results of an audit of second evacuations. in the treatment of molar pregnancy and shows that the procedure is rarely of benefit when the hCG level is >1500IU/L. The figure show the number of patients who required chemotherapy after their second evacuation.
Assessment and hCG surveillance
Following diagnosis patients should be registered and followed by serial serum hCG levels. For confirmed partial moles patients will be monitored with serum and urine samples every 2 weeks until hCG levels are normal. Once confirmed with a normal sample four weeks later, follow up will be complete. For complete moles if the hCG falls to normal within 8 weeks of evacuation the monitoring can be stopped at 6 months post evacuation. If the hCG falls more slowly, monitoring can stop at 6 months after the first normal value. After normalisation of the serum hCG the monitoring is by urine hCG monthly.
The role of hCG in trophoblast disease diagnosis and management
Produced predominantly by the syncytiotrophoblast cells, hCG is an glycosylated heterodimer protein consisting of the non-covalently bonded alpha and beta units. Whilst in pregnancy the hCG molecule is intact and full size, in malignant disease a number of variants can occur including; hyperglycosylated hCG, nicked hCG, hCG missing the beta subunit C terminal peptide and the free beta subunit. With the exception of a few atypical cases of PSTT, hCG is always expressed by malignant trophoblast cells. The measurement of the hCG level allows an estimation of the number of proliferating cells, forms an key part of the assessment of the patients disease risk and provides the simplest method following the response to treatment.
In the absence of tumour hCG production the serum half life of hCG is 24-36 hours, however in the clinical situation total hCG levels characteristically show slower falls as the tumour cells continue to produce some hCG whilst their number decreases with treatment.
Advice to patients regarding Contraception during the monitoring phase
Oestrogen and/or progestogens taken between evacuation of the mole and return to normality of hCG values appear NOT to increase the risk of invasive mole or choriocarcinoma developing. Therefore, women may use oral contraceptives after molar evacuation, before hCG returns to normal. Pregnancy should be avoided until after the completion of the surveillance period.
CXH Molar Pregnancy Indications for chemotherapy treatment during surveillance
- Brain, liver, GI mets or lung mets >2cm on CXR
- Histological evidence of choriocarcinoma
- Heavy PV bleeding or GI/intraperitoneal bleeding
- Pulmonary, vulval or vaginal mets unless the hCG level is falling
- Rising hCG in two consecutive serum samples
- hCG > 20,000 IU/L more than 4 weeks after evacuation
- hCG plateau in 3 consecutive serum samples
- Raised hCG level 6 months after evacuation (even if falling)
Patients in this last group are reviewed at CXH and individualised decisions are made re treatment or further observation.
FIGO Indications for chemotherapy treatment
- hCG plateau of 4 values +/- 10% over a 3 week period
- hCG increase of >10% of three values over a 2 week period
- Persistence of hCG for more than 6 months after molar evacuation.
CXH Initial assessment at admission
For patients admitted for treatment after a documented molar pregnancy
- Full history to include: Details of the antecedent and all other pregnancies, LMP date, evacuation date and method, OCP usage, bleeding and other symptoms particularly respiratory and CNS.
- Investigations: FBC, biochem, clotting, HIV, HBV serology, hCG serum levels are measured twice a week during treatment, Group and Save.
- Doppler Ultrasound of the pelvis to confirm disease presence and volume and to rule out the possibility of a new pregnancy and CXR.
For patients admitted for treatment for presumed choriocarcinoma or PSTT
- As above plus
- CT scan thorax, abdomen and liver
- MRI brain scan
- Diagnostic CSF hCG level if lung or brain metastases,
- GFR prior to EP/EMA or CNS EMA/CO chemo
Prognostic factors and treatment groups
Data from the early days of chemotherapy treatment for trophoblast disease shows clearly that there is a relationship between the level of elevation of hCG at presentation, the presence of distant metastases and the reducing chances of cure with single agent chemotherapy. This relationship and the impact on treatment choice and cure rate was first codified at Charing Cross Hospital with the Bagshawe scoring system published in 1976 (Bagshawe 1976).
Subsequently there have been a number of revisions and parallel systems introduced that are broadly similar to this original. In the revised 2000 FIGO prognostic score table is shown below.
From these parameters, an estimate of the risk category can be obtained and patients offered initial treatment either with single agent chemotherapy if their score is 6 or less or multi-agent combination chemotherapy for scores of seven and over (FIGO 2002).
WHO/FIGO scores
Low risk 0-6
High risk >7